Mon - Fri 10am - 10pm
Sat- Sun 10am - 7pm
hello@nightwatchuc.com
2118 Pleasant Valley Road Winchester, VA 22601
(540) 545-9999
blog spot
The
Health hub
A collection of helpful articles & information to spread awareness through education from our staff to you
When your child is sick or hurt, the best place to go depends on two things: how severe the symptoms are and how fast your child needs to be evaluated. If you’re seeing emergency warning signs (trouble breathing, severe allergic reaction, seizure, or a child who is hard to wake), skip the debate and go straight to the ER or call your local emergency number.
Below is a practical, parent-friendly guide to help you decide.
Choose the ER if your child may be in danger right now or could worsen quickly.
Choose Urgent Care if your child needs same-day evaluation for a non-life-threatening problem (especially when your pediatrician is closed or can’t see you soon).
Choose the Pediatrician for routine care, ongoing concerns, and problems that can safely wait for an office visit.
If you’re unsure, many urgent care clinics also offer telemedicine or nurse/triage guidance—but if your gut says “this is an emergency,” trust that and go to the ER.
Go to the ER now (or call emergency services) if…
These are red-flag symptoms that should be treated as emergencies:
- Trouble breathing, fast breathing, ribs pulling in with breaths, blue/gray lips or face.
- Severe allergic reaction: facial/lip/tongue swelling, trouble breathing, widespread hives with vomiting or dizziness.
- Seizure, fainting, or your child is very hard to wake/confused.
- Head injury with loss of consciousness, repeated vomiting, worsening headache, or unusual behavior.
- Severe bleeding that won’t stop with firm pressure.
- Suspected broken bone with deformity (bone looks out of place), severe pain, or numbness/tingling.
- Severe dehydration: no urine for 8–12 hours, very dry mouth, no tears, lethargy, or sunken eyes (especially in babies).
- Fever in a baby under 3 months (or any infant who looks very ill).
- Poisoning/ingestion (medications, chemicals, unknown substances), or concern for overdose.
- Severe abdominal pain, especially with a hard belly, persistent vomiting, or pain in the lower right abdomen.
- Any situation where you feel your child is not safe to wait.
Urgent Care is usually best for…
Urgent care is a strong option when your child needs prompt care but is stable.

Why parents choose urgent care: Urgent care is a go-to option when you need your child seen the same day but your pediatrician is fully booked. Many urgent care clinics can also provide on-site testing, like rapid strep, flu, or COVID tests, and may offer X-rays, which can speed up answers and treatment decisions. It’s also especially helpful during evenings and weekends when your pediatrician’s office is closed, so you’re not forced to wait until the next business day.
Your Pediatrician is best for… Your child’s pediatrician should be your home base for routine and long-term care, including well visits, vaccines, and growth and developmental check-ins. They’re also the best fit for ongoing or recurring concerns, like asthma management plans, eczema, constipation, and repeated ear infections, because they can follow patterns over time and adjust care as your child grows. Pediatricians are ideal for behavior and sleep concerns, school-related issues, anxiety, and ADHD evaluations, and they’re a great choice when symptoms are mild, improving, and safe to wait for an appointment. They should also handle follow-ups after urgent care or ER visits to make sure your child is recovering well and to coordinate next steps if anything needs closer monitoring. Why it matters: your pediatrician knows your child’s history, tracks progress across multiple visits, and can coordinate referrals to specialists when needed.
Common scenarios (where to go)
1) Ear pain + low fever
- Usually urgent care or pediatrician (same/next day).
- ER only if severe swelling behind the ear, stiff neck, extreme lethargy, or severe dehydration.
2) Sore throat + fever
- Urgent care or pediatrician for strep testing and guidance.
- ER if trouble breathing, drooling with inability to swallow, or signs of dehydration.
3) Asthma/wheezing
- Urgent care if mild–moderate and improving with rescue inhaler.
- ER if your child is struggling to breathe, can’t speak in full sentences (age-appropriate), lips look bluish, or rescue meds aren’t helping.
4) Cut on the face
- Urgent care is often ideal, especially if it needs stitches and it’s within a few hours of the injury.
- ER if bleeding won’t stop, the wound is deep with visible fat/muscle, or there’s concern for a head injury.
5) Head bump after a fall
- Urgent care if your child is acting normal and symptoms are mild.
- ER for loss of consciousness, repeated vomiting, worsening headache, confusion, seizure, or very abnormal sleepiness.
If you’re stuck between urgent care and the ER, choose the safer option—especially for breathing problems, dehydration, head injuries, or very young infants. And if you’re deciding between urgent care and the pediatrician, urgent care makes sense when you can’t get a timely appointment or symptoms are worsening.
For same-day urgent care in Winchester, come to 2118 Pleasant Valley Road, Winchester, VA 22601, or call (540) 545-9999 and we’ll help you decide whether you should come in or use a virtual visit.
CATEGORY
2/22/2026
POSTED
Measles is appearing in more communities across the U.S., and many parents are understandably concerned. While measles may feel like an illness from the past, it remains one of the most contagious viral infections affecting children today — and it often begins in a way that’s easy to miss.
At Night Watch Urgent Care, our pediatric team is hearing the same questions from families every day:
How does measles start? How worried should I be? And when should I bring my child in?
This guide is designed to give parents clear, practical information so you can recognize symptoms early, understand how measles spreads, and feel confident about next steps if your child becomes ill.
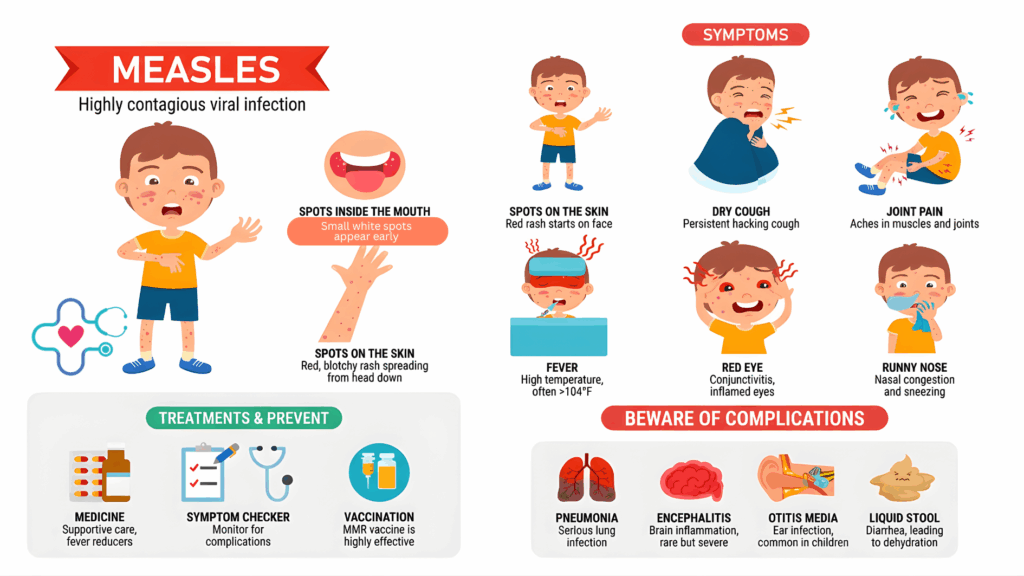
What Is Measles and Why Is It So Contagious?
Measles is a viral illness that spreads through the air when an infected person coughs, sneezes, or breathes. Unlike many other childhood viruses, measles does not require close contact to spread.
The virus can remain in the air for up to two hours after an infected person leaves a room, meaning exposure can occur in classrooms, daycare centers, grocery stores, or medical offices without direct interaction.
What makes measles especially challenging is that children are contagious before parents realize it’s measles. By the time the classic rash appears, the virus may have already spread to others.
This is why early recognition and prevention play such an important role in protecting families and communities.
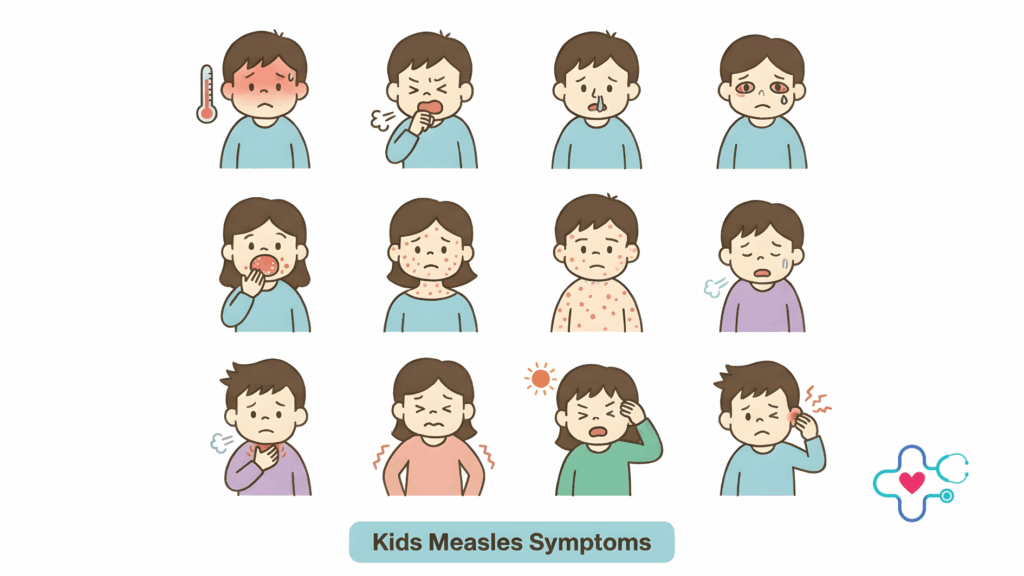
Early Measles Symptoms Parents Often Miss
Many parents associate measles with a rash — but the rash comes later.
In the early stage, measles often looks like a severe cold or flu. Symptoms may include:
- High fever, often rising quickly
- Cough
- Runny nose
- Red, watery, or irritated eyes
- Fatigue, irritability, or decreased appetite
Because these symptoms are common with many viral illnesses, measles can be difficult to identify at first. A key difference parents often notice is how sick their child looks and feels, especially when fever is high and persistent.
When the Rash Appears
The measles rash typically develops three to five days after fever begins. It usually:
- Starts on the face or hairline
- Spreads downward to the neck, trunk, arms, and legs
- Appears as flat red spots that may merge together
If your child develops fever followed by a spreading rash, or symptoms seem to worsen instead of improve, it’s important to contact a medical provider.
Why Measles Can Be Serious for Children
While many children recover from measles, it is not always a mild illness. Some children are at higher risk for complications, including:
- Infants under 12 months
- Children who are not fully vaccinated
- Children with asthma or chronic medical conditions
- Pregnant individuals and immunocompromised family members
Complications can include ear infections, dehydration, pneumonia, and in rare cases, serious neurologic issues. This is why prompt guidance and careful monitoring are important, even if symptoms seem manageable at first.
How Parents Can Protect Their Children From Measles
MMR Vaccination
The MMR (measles, mumps, rubella) vaccine is the most effective way to prevent measles. Two doses provide strong, long-lasting protection and significantly reduce the risk of severe illness and complications.
If you’re unsure whether your child is up to date on vaccinations or have questions about timing, a pediatric provider can help review your child’s immunization history and answer concerns.
Reducing Exposure
During times of increased measles activity:
- Avoid close contact with anyone who has fever and rash symptoms
- Be cautious in crowded indoor settings when possible
- Notify your healthcare provider if your child may have been exposed
Protecting High-Risk Family Members
If your household includes infants, pregnant individuals, or people with weakened immune systems, extra care is important. Keeping eligible family members vaccinated and limiting exposure to illness helps protect those most vulnerable.
When to Call Before Coming In
Because measles spreads so easily, calling ahead before visiting urgent care is essential.
Please contact a medical provider first if your child has:
- Fever along with a rash
- Known exposure to someone with measles
- Symptoms and is not fully vaccinated
Calling ahead allows our team to prepare appropriately and helps protect other children and families in our care.
Seek urgent or emergency care immediately if your child experiences:
- Trouble breathing or fast, labored breathing
- Extreme sleepiness, confusion, or difficulty staying awake
- Signs of dehydration such as very dry mouth, no tears, or minimal urination
- A very high fever that does not respond to medication
You never have to make these decisions alone. We are always here to help guide you.
Parents searching for measles treatment in Winchester can visit Night Watch Urgent Care for timely pediatric assessment and guidance.
We help families decide whether symptoms can be monitored safely at home or require in-person evaluation, while keeping safety and infection control a priority.
CATEGORY
2/06/2026
POSTED
Why Kids in the Kitchen = Burns, Cuts & Urgent Care Visits
Your 7-year-old: “Can I help make dinner?”
You: “Sure! You can stir the pasta.”
Five minutes later: They grabbed the hot pot handle. With their bare hand.
Now you’re at Night Watch.
Why Kids Get Hurt in the Kitchen
Children LOVE helping in the kitchen. They also:
- Don’t understand cause and effect yet
- Move unpredictably
- Have poor impulse control
- Forget instructions immediately
- Get excited and rush
- Touch things they’re told not to touch
Translation: They’re injury magnets.
The Most Common Kid Kitchen Injuries
1. Burns (Top of the List)
🍳 Hot pots and pans
Kid reaches for something, touches hot cookware. Second-degree burns on palms/fingers.
💧 Boiling water
Spills, splashes, or they pull pot handle. Scalding burns on hands, arms, chest.
🔥 Stove burners
“I didn’t know it was still hot.” Electric burners stay hot for LONG time after turning off.
🍕 Ovens
Reaching in, arm touches rack or door. Burns in stripes across forearm.
2. Cuts
🔪 Knife accidents
“I was just trying to help cut the vegetables.” Deep lacerations on fingers.
🥫 Can lids
Sharp edges on opened cans. Kids don’t realize how sharp they are.
🍷 Broken glass
Drop a glass, try to pick it up. Lacerations on hands.
3. Other Injuries
- Fingers smashed in drawers/cabinets
- Falls from standing on chairs/stools
- Slipping on spills
- Getting hit by falling pots/utensils
When to Bring Them to Night Watch
For Burns:
- Blisters larger than a quarter
- Burns on face, hands, feet, or genitals
- White or charred skin
- Child is in severe pain
- Burn larger than child’s palm
For Cuts:
- Won’t stop bleeding after 10 minutes
- Deep cut (gaping edges)
- On face, hands, or over joints
- Child can’t move fingers normally
- Numbness or tingling
What We Do at Night Watch
We specialize in pediatric care. We know how to:
- Keep kids calm during treatment
- Properly assess burn depth in children
- Apply child-friendly dressings
- Give age-appropriate pain relief
- Educate parents on wound care
Teaching Kitchen Safety
Before they help in the kitchen:
The Rules (Repeat Often)
- “Hot means DON’T TOUCH”
- “Knives are not toys”
- “Ask before touching anything”
- “If you drop something, tell a grown-up”
- “Walk, don’t run in the kitchen”
Safe Tasks by Age
Ages 2-4:
- Washing produce, tearing lettuce, mixing cold ingredients
Ages 5-7:
- Measuring, pouring, stirring, setting table, using butter knife
Ages 8-10:
- Peeling vegetables, using microwave, cracking eggs, using hand mixer
Ages 11+:
- Using sharp knives WITH SUPERVISION, basic stove use, following recipes
Creating a Safer Kitchen
- Turn pot handles inward (away from edge where kids can grab)
- Use back burners when possible
- Keep sharp objects in drawers/cabinets kids can’t reach
- Store cleaning products up high or locked
- Teach safe knife handling (claw grip, cut away from body)
- Supervise constantly — they’re quick!
First Aid at Home
For Minor Burns:
- Run under cool (not ice cold) water for 10-20 minutes
- Cover with clean, dry cloth
- Give age-appropriate pain relief
- Don’t pop blisters
For Minor Cuts:
- Apply direct pressure for 10 minutes
- Clean with soap and water
- Apply antibiotic ointment
- Cover with bandage
👨🍳 “I can help!” (Famous last words before urgent care)
We’ll patch them up and teach you safer cooking.
CATEGORY
1/31/2026
POSTED
Why Your Kid’s Eyes (and Head) Can’t Take It Anymore
7:30 AM: Your kid logs onto their school Chromebook.
3:30 PM: School’s out. They immediately grab their phone.
5:00 PM: Homework. Back to the Chromebook.
7:00 PM: Gaming with friends. Xbox, PlayStation, Switch, or PC.
9:00 PM: “I have a headache. My eyes hurt.”
No kidding.
The Screen Time Reality for Kids
Let’s add it up:
- School: 6-7 hours on school-issued devices
- Homework: 1-2 hours on computers/tablets
- Gaming/YouTube/Social Media: 2-4 hours
- TOTAL: 9-13 hours per day
Their eyes are working non-stop from morning until bedtime.
And we wonder why they have headaches.
What Happens to Kids’ 👁️
Children’s eyes are still developing. They’re more vulnerable to screen-related strain.
Digital Eye Strain in Kids
Same as adults, but worse:
- 😫 Eye fatigue and discomfort
- 🤕 Headaches (forehead, temples, behind eyes)
- 💧 Dry, irritated eyes
- 🌫️ Blurry vision
- 💢 Neck and shoulder pain
- 😴 Trouble sleeping (blue light disruption)
Myopia (Nearsightedness) Risk
Studies show excessive screen time + lack of outdoor time = increased myopia risk.
Nearsightedness in children has doubled in the last 30 years. Screen time is a major factor.
🎮 The Gaming Problem
Gaming is particularly hard on eyes:
- Fast-moving graphics = constant rapid eye movements
- Intense focus = reduced blinking
- Close screen distance = maximum eye strain
- Extended sessions = no breaks
- Poor posture = neck/shoulder/head pain
Add school screen time on top? Recipe for headaches.
What Parents Can Do
The 20-20-20 Rule
Every 20 minutes, look at something 20 feet away for 20 seconds.
For gaming: Set a timer. Take breaks between matches/levels.
Screen-Free Time
- 1 hour before bed: No screens (helps sleep)
- Meals: Screen-free family time
- After school: 30-60 min outdoor time before homework
Proper Setup
- Screen 20-26 inches away from eyes
- Top of screen at or below eye level
- Room lighting matches screen brightness
- Reduce glare (anti-glare screens, adjust window blinds)
Blue Light Filters
Enable “night mode” on all devices. Especially important 2-3 hours before bed.
Outdoor Time
90+ minutes of outdoor time daily reduces myopia risk. Eyes need to focus on distant objects.
When to Come to Night Watch
Bring your child in if:
- Frequent headaches interfering with school
- Squinting or sitting very close to screens
- Complains of blurry vision
- Eye pain (not just tired eyes)
- Red, swollen, or persistently dry eyes
- Double vision or seeing halos around lights
- Sudden vision changes
We can evaluate and refer to pediatric optometry if needed.
Do They Need Glasses?
Sometimes “screen headaches” are actually undiagnosed vision problems.
Signs they might need an eye exam:
- Headaches when reading or doing homework
- Holds devices very close to face
- Complains words look blurry
- Loses place when reading
- Avoids reading or screen work
Setting Realistic Limits
We know you can’t eliminate school screen time. But you can control recreational time:
- Set gaming time limits (1-2 hours max)
- Enforce screen-free zones (bedrooms, dinner table)
- Encourage non-screen activities
- Model good behavior (you’re on screens too much too)
🎮 School all day. Gaming all night. Headaches all the time.
Let’s figure out if it’s just screen overload – or something more.
CATEGORY
1/29/2026
POSTED
Why Your Child’s Immune System Needs This Many Germs
Your toddler just recovered from a cold.
They went back to daycare Monday morning.
By Thursday, they have a fever again.
You want to scream.
We get it. We see this constantly. And we have good news:
This is exactly what’s supposed to happen.
Your Child’s Immune System: The First 5 Years
Here’s what most parents don’t realize:
Babies are born with an immature immune system. It has to learn what’s dangerous and what’s not. And the only way it learns is through exposure.
Think of it like learning to read:
Year 1-2: Learning the alphabet (basic immune responses)
Year 3-4: Sounding out words (recognizing more viruses)
Year 5-6: Reading fluently (strong immune memory)
You can’t skip steps. They have to go through it.
🦠 The Germ Library
Every time your child gets sick, their immune system is building a “library” of how to fight that specific germ.
First Exposure
Body encounters new virus → Immune system scrambles to figure out how to fight it → Takes 7-10 days → Child is sick the whole time
Second Exposure (Same Virus)
Body recognizes virus immediately → Immune response is faster and stronger → Illness is shorter or prevented entirely
The problem? There are 200+ viruses that cause the common cold alone. Plus flu viruses, stomach bugs, RSV, hand-foot-mouth disease, pink eye viruses…
They have to catch them all.
What’s Actually Normal
By Age:
Infants (0-12 months)
6-8 colds per year (especially if siblings or daycare)
Toddlers (1-3 years)
8-12 illnesses per year (this is the WORST stage)
Preschool (3-5 years)
6-10 illnesses per year (starting to improve)
School-Age (5+ years)
4-6 illnesses per year (finally calming down)
Translation: If your 3-year-old gets sick once a month, that’s textbook normal.
👶 The Daycare Effect
Kids in daycare get sick 50-100% more than kids at home.
The first year of daycare is brutal:
- Expect to be sick a lot
- Expect to use all your sick days
- Expect your child to bring home every germ imaginable
- Expect YOU to catch half of it
But here’s the upside:
Kids who go to daycare early get sick MORE in the first few years but LESS once they hit elementary school. Kids who stay home get sick LESS early but MORE when they start kindergarten.
Either way, they’re catching the same germs. Just different timing.
When It’s NOT Normal
Come see us if:
- 2+ pneumonias in one year
- 4+ ear infections requiring antibiotics in one year
- Infections that don’t respond to standard treatment
- Poor growth or failure to gain weight
- Chronic diarrhea lasting weeks
- Deep skin abscesses or unusual infections
Lots of colds = normal. Repeated serious infections = not normal.
How We Help at Night Watch
When they’re sick (again):
- Quick diagnosis (strep, flu, RSV, ear infection, etc.)
- Age-appropriate treatment
- Evaluate pattern of illness
- Reassure worried parents (we do this a LOT)
- Refer for immune testing if truly warranted
💪 Building Strong Immunity
What you CAN do:
- Good nutrition (variety of fruits, vegetables, proteins)
- Adequate sleep for their age
- Keep vaccines up to date
- Hand washing (won’t prevent everything, but helps)
- Don’t stress—chronic stress weakens immunity
What WON’T help:
- Immune-boosting supplements (mostly marketing)
- Excessive sanitizing (some germ exposure is good)
- Keeping them home from all activities (defeats the purpose)
They’re sick again. Their immune system is working. We promise.
CATEGORY
1/22/2026
POSTED
“Pink Eye Going Around—AGAIN!”
You see the notification on your phone:
“FYI – multiple cases of pink eye in Mrs. Johnson’s class.”
Your heart sinks. Your kid is in Mrs. Johnson’s class.
Sure enough, the next morning: “Mom, my eye feels weird.”
Here we go again.
📚 Why Schools Are Pink Eye Breeding Grounds
January = peak pink eye season in schools. Here’s why:
- Back from winter break – mixing germ pools from different families
- Cold/flu season – viral pink eye often accompanies colds
- Indoor classroom time – less fresh air, more shared surfaces
- Kids touching EVERYTHING – then rubbing their eyes
- Close contact – circle time, group projects, lunch tables
One infected kid can spread pink eye to half the class in days.
What Parents Need to Know
It Looks Different Depending on the Type
VIRAL (most common in school outbreaks):
- Watery, clear tears
- Very red, very itchy
- Usually starts one eye, spreads to other
- May have runny nose, sore throat
BACTERIAL (needs antibiotics):
- Thick, goopy, yellow-green discharge
- Eyes crusted shut in morning
- More painful than viral
- Can spread to other eye
When to Bring Your Child to Winchester
Come in if:
- Eyes are red and producing discharge
- School requires doctor’s note before return
- Thick, colored goop (likely bacterial)
- Child complains of eye pain
- Vision seems blurry or affected
- Not improving after 3 days
- Infant or baby has pink eye (always needs evaluation)
What We Do at Night Watch
We specialize in pediatric care, and we see pink eye constantly this time of year:
- Quick examination to determine viral vs. bacterial
- Antibiotic eye drops if bacterial (prescribed on-site)
- School clearance notes so they can return
- Parent education on preventing spread to siblings
- Comfort measures for itchy, irritated eyes
🏠 Keeping It from Spreading at Home
You have multiple kids. How do you keep them ALL from getting it?
- Separate towels & pillows
- Wash hands constantly – especially after touching infected child’s face
- Change pillowcase daily
- Don’t let them share devices/tablets
- Disinfect high-touch surfaces – doorknobs, light switches, bathroom faucets
- Teach “don’t touch your eyes” (good luck)
- Wash infected child’s hands frequently
👶 Pink Eye in Babies
Infants with pink eye always need medical evaluation.
Why? Pink eye in newborns can indicate:
- Blocked tear duct (common, usually harmless)
- Bacterial infection (needs prompt treatment)
- In rare cases, serious infection requiring immediate care
If your baby (under 1 year) has red, goopy eyes, bring them in same day.
📅 When Can They Go Back to School?
Most schools require:
Bacterial pink eye: 24 hours after starting antibiotic drops + doctor’s note
Viral pink eye: When discharge has stopped and eyes are no longer red
We provide school clearance notes at your visit.
💡 Home Care Tips
While waiting for it to clear:
- Warm compress – helps loosen crusty discharge
- Gently wipe away discharge with clean, damp cloth (use once, wash)
- Cool compress – for itching relief
- No contact lenses until completely healed
- Skip eye makeup (and throw out old mascara after infection)
👁️ Pink eye is going around. We’ve seen it before. Get them diagnosed. Get them back to school.
CATEGORY
1/20/2026
POSTED
Why Your Kid’s Humidifier Is Still Making Them Sick
Your child has been coughing for two weeks.
Not all day – mostly at night. And in the morning. They wake up wheezing. Their chest sounds tight. They say it’s hard to breathe.
You’ve tried everything: cough medicine, honey, propping up their pillow. Nothing helps.
Then someone asks: “Do you run a humidifier in their room?”
Yes. Of course you do. The air is so dry. You’re trying to help.
“When’s the last time you cleaned it?”
…Oh.
🫁 How Dirty Humidifiers Affect Kids’ Lungs
Children’s respiratory systems are more vulnerable than adults’:
- Smaller airways = easier to inflame and obstruct
- Still-developing immune systems = less able to fight respiratory infections
- Breathe faster = inhale more contaminated air per breath
- Sleep in small rooms = higher concentration of airborne contaminants
When a humidifier sprays bacteria, mold spores, and mineral dust into the air, kids’ lungs take the biggest hit.
What We Seeing at Night Watch
Child comes in with:
- Persistent nighttime cough
- Wheezing
- Shortness of breath
- Sometimes fever
We test for flu, RSV, COVID – all negative. No strep. Lungs sound clear-ish. Oxygen levels normal.
Then we ask: “Do you run a humidifier?”
Almost always: Yes.
“When did you last clean it?”
Usually: Silence. Or “Um… a few weeks ago?”
Symptoms of Humidifier-Related Illness
Come to Night Watch if your child has:
- Nighttime cough that’s been going on for days/weeks
- Wheezing or difficulty breathing
- Complaints of chest tightness
- Symptoms worse at night, better during school
- Fever with respiratory symptoms
- Asthma suddenly harder to control
- Recurring respiratory infections
🫧 “But I Rinse It Every Week!”
Here’s the problem: rinsing isn’t cleaning.
What you need to do:
Daily
- Empty ALL water from tank and base
- Rinse thoroughly with clean water
- Dry with clean towel (don’t just refill wet tank)
Every 3 Days
- Fill tank with white vinegar
- Let sit 20-30 minutes
- Scrub with brush to remove mineral deposits
- Rinse thoroughly
Weekly
- Disinfect with 3% hydrogen peroxide OR diluted bleach (1 tsp per gallon water)
- Let sit 10-30 minutes
- Rinse VERY thoroughly (no chemical residue)
Always
- Use distilled or demineralized water ONLY
- Replace filters per manufacturer instructions
🔬 The Science: What’s Growing
Research shows dirty humidifiers harbor:
- Legionella bacteria (causes Legionnaires’ disease)
- Pseudomonas aeruginosa (respiratory infections)
- Mold spores (asthma triggers, allergic reactions)
- Endotoxins (inflammatory compounds)
- Mineral particles (lung irritation)
All of this gets turned into a fine mist and sprayed directly into your child’s face while they sleep.
What We Do at Night Watch
- Evaluate respiratory symptoms
- Rule out infections (flu, RSV, COVID, pneumonia)
- Provide breathing treatments if needed
- Assess for environmental triggers
- Give parents concrete steps to eliminate exposure
The Experiment
Try this:
- Deep clean your humidifier (or throw it out and buy a new one)
- OR stop using it entirely for one week
- See if symptoms improve
If your child’s cough gets better when the humidifier is off? That’s your answer.
Sometimes the solution is simpler than you think.
CATEGORY
1/16/2026
POSTED
When Holiday Pet Excitement Leads to Urgent Care
You got your kids the puppy they’ve been begging for. Christmas wish granted!
Day 1: Pure joy. Day 2: Lots of energy. Day 3: “Mom, the puppy bit me!”
You look at your child’s hand. There are teeth marks. It broke the skin. It’s starting to swell.
Wait… do puppies bite this much? Is this normal? Should you be worried?
Why Kids Get Bitten More
Here’s what most parents don’t realize: children are more likely to get bitten or scratched by pets than adults.
Why?
- They move unpredictably (running, jumping, shrieking with excitement)
- They’re at face level with small dogs and puppies
- They don’t read warning signs (ears back, growling, stiff body)
- They want to hug and squeeze (which animals often don’t like)
- They put their hands where puppies bite during play
And puppies? They explore everything with their mouths. Including your child.
When to Bring Your Child to Night Watch
Come in right away if:
- The bite or scratch broke the skin
- It’s on their face, hands, or near joints
- It’s a puncture wound (deep, narrow)
- Bleeding won’t stop after 10 minutes of pressure
- Signs of infection (redness, swelling, warmth, pus)
- You’re not sure if the pet is fully vaccinated
🐱 Cat Scratches: Tiny But Trouble
Got a kitten instead? Those needle-sharp claws can cause Cat Scratch Disease.
What is it? Bacterial infection from bacteria in cat saliva that gets on their claws. Can cause fever, swollen lymph nodes, and fatigue in children.
Symptoms appear 3-14 days after the scratch:
- Red bump or blister at scratch site
- Swollen lymph nodes (especially under arms or neck)
- Fever
- Your child feeling tired or unwell
Cat scratches need treatment. Don’t ignore them.
Teaching Kids to Be Safe with New Pets
Prevention is key. Teach your children:
- “Gentle hands” No pulling, grabbing, or squeezing
- “No face kisses” Keep faces away from puppy mouths
- “Let sleeping pets lie” Don’t wake or startle them
- “No hands in mouth” Use toys for play, not fingers
- “Back away if scared” If the pet seems upset, give space
- “Tell a grown-up” Always report bites/scratches immediately
How We Help at Night Watch
At Night Watch, we treat animal bites and scratches in children regularly:
- Gentle, thorough wound cleaning
- Child-friendly evaluation (checking for nerve/tendon damage)
- Stitches if needed (with numbing medicine first)
- Antibiotics to prevent infection
- Parent education on wound care and pet safety
🏡 What to Do at Home Immediately
If your child gets bitten or scratched:
- Wash the wound immediately with soap and running water (5+ minutes)
- Apply pressure if bleeding
- Don’t panic (it scares your child more)
- Bring them to Night Watch for proper evaluation
🐾 New pets + excited kids = occasional injuries. We’re here when it happens.
CATEGORY
1/13/2026
POSTED
When Teen Exhaustion Goes Beyond Normal
You’ve heard “I’m tired” so many times you’ve lost count.
Morning, afternoon, evening – doesn’t matter. Your teen is exhausted.
At first, you figured it was January. Back to school after winter break is always rough. But it’s been weeks now, and if anything, they’re getting worse.
You’re starting to worry. Should you be worried?
🤔 Trust Your Gut
As a parent, you know your kid. You know their energy levels, their mood, their “normal.”
And right now? This doesn’t feel normal.
Here’s the thing: you’re probably right.
When exhaustion is severe enough that you’re Googling it, questioning it, losing sleep over it – that’s your parental instinct telling you something’s off.
🚨 Signs This Isn’t “Just Teen Tiredness”
- They’re sleeping 10-12+ hours and still exhausted
- Can’t wake up for school even with multiple alarms
- Falling asleep in class, during homework, while watching TV
- Stopped doing activities they used to love
- Withdrawing from friends and family
- Grades suddenly dropping
- Other symptoms (sore throat, pale skin, weight changes, mood shifts)
If you’re seeing several of these? Time to get them checked.
🩺 What Parents Should Know
Extreme exhaustion in teens is often a symptom of something treatable:
😷 Mononucleosis (“Mono”)
Most common in teens.
Causes: Extreme fatigue (lasting weeks), sore throat, swollen lymph nodes, fever. Spread through saliva – shared drinks, kissing, even sharing food.
🩸 Anemia (Low Iron)
Especially common in teenage girls.
Causes: Constant tiredness, pale skin, shortness of breath, dizziness, cold hands/feet. Often related to menstruation or diet.
Thyroid Issues
More common in teen girls than you’d think.
Causes: Overwhelming fatigue, weight gain, feeling cold all the time, dry skin, “brain fog,” difficulty concentrating.
💤 Sleep Disorders
Sleep apnea, insomnia, restless leg syndrome.
Causes: Sleeping for hours but waking up exhausted, snoring, gasping during sleep, never feeling rested.
😔 Depression or Anxiety
Mental health = physical symptoms.
Causes: Crushing fatigue, loss of interest in everything, withdrawal, changes in appetite, overwhelming sadness or worry.
🍔 Nutritional Deficiencies
Vitamin D, B12, and other deficiencies.
Causes: Fatigue, weakness, difficulty concentrating. Common in teens who skip meals or follow restrictive diets.
💙 How We Help at Night Watch
At Night Watch, we specialize in pediatric and adolescent care. We understand that teens aren’t just “small adults” – their bodies and brains work differently.
We can:
- Run comprehensive blood work (mono, anemia, thyroid, vitamins)
- Conduct thorough physical exams
- Screen for mental health concerns
- Provide treatment or specialist referrals
- Answer all your worried-parent questions
Most importantly: we take your concerns seriously.
📅 When Should You Come In?
Don’t wait until it’s “bad enough.” Come in if:
- Exhaustion has lasted more than 2 weeks
- It’s affecting their school performance or social life
- They have other symptoms
- They’ve stopped doing things they used to enjoy
- Your gut tells you something’s wrong
You know your child better than anyone. If something feels off, trust that instinct.
Your worry isn’t an overreaction. It’s good parenting. Let’s figure out what’s going on together.
CATEGORY
1/09/2026
POSTED
Food Poisoning in Kids: Why They Get Sicker, Faster
It’s January. You’re cleaning out the fridge. Your kid wanders in, opens a container of leftover turkey, and before you can say “Wait, how old is that?”—they’ve already eaten half of it.
Two hours later: vomiting. Four hours later: diarrhea. Six hours later: you’re Googling “is this food poisoning?”
Yes. Yes it is.
Why Kids Get Hit Harder
Children are more vulnerable to food poisoning than adults because:
- Their immune systems are still developing
- They have less stomach acid to kill bacteria
- They dehydrate faster due to smaller body size
- They can’t always tell you how bad they feel
What might be “rough but manageable” for an adult can become a medical emergency for a child within hours.
Signs Your Child Needs Urgent Care NOW
Don’t wait it out. Bring them in if you see:
- 🤢 Vomiting for more than 12 hours
- 💧 Can’t keep any liquids down
- 💩 Diarrhea with blood or mucus
- 🥵 Fever over 100.4°F (infants) or 102°F (older kids)
- 😴 Extreme lethargy or won’t wake up properly
- 😭 Crying without tears
- 👄 Dry mouth, cracked lips, sunken eyes
- 🚽 No wet diapers in 6+ hours (babies) or no urination in 8+ hours (older kids)
- 😖 Severe stomach pain that makes them double over
Dehydration: The Real Danger
Most kids recover from food poisoning just fine—if they stay hydrated.
But when they’re vomiting and having diarrhea, they lose fluids fast. And small children don’t have much to spare.
Signs of dehydration in kids:
- Decreased energy or activity level
- No tears when crying
- Sunken soft spot on baby’s head
- Dry, sticky mouth
- Dark yellow or very little urine
If you see these signs, don’t try to “wait and see.” Come to Night Watch.
What We Do
We specialize in pediatric care, and we see food poisoning cases regularly. Here’s how we help:
- IV fluids to rehydrate quickly and safely
- Anti-nausea medication so they can keep liquids down
- Stool testing if we suspect bacterial infection
- Antibiotics (when appropriate—not all food poisoning needs them)
- Parent guidance on recovery and when to follow up
Common Culprits in Kids
- Leftover poultry (turkey, chicken): Salmonella
- Deli meats or hot dogs: Listeria
- Egg dishes (quiche, casseroles): Salmonella
- Dairy products left out: Staph bacteria
- Undercooked ground beef: E. coli
How Long Until They’re Better? ⏰
Most food poisoning resolves in 24-48 hours with proper hydration and rest.
But: Some bacterial infections can last longer and kids can take longer to bounce back than adults.
CATEGORY
1/06/2026