Mon - Fri 10am - 10pm
Sat- Sun 10am - 7pm
hello@nightwatchuc.com
2118 Pleasant Valley Road Winchester, VA 22601
(540) 545-9999
blog spot
The
Health hub
A collection of helpful articles & information to spread awareness through education from our staff to you
Measles is appearing in more communities across the U.S., and many parents are understandably concerned. While measles may feel like an illness from the past, it remains one of the most contagious viral infections affecting children today — and it often begins in a way that’s easy to miss.
At Night Watch Urgent Care, our pediatric team is hearing the same questions from families every day:
How does measles start? How worried should I be? And when should I bring my child in?
This guide is designed to give parents clear, practical information so you can recognize symptoms early, understand how measles spreads, and feel confident about next steps if your child becomes ill.
What Is Measles and Why Is It So Contagious?
Measles is a viral illness that spreads through the air when an infected person coughs, sneezes, or breathes. Unlike many other childhood viruses, measles does not require close contact to spread.
The virus can remain in the air for up to two hours after an infected person leaves a room, meaning exposure can occur in classrooms, daycare centers, grocery stores, or medical offices without direct interaction.
What makes measles especially challenging is that children are contagious before parents realize it’s measles. By the time the classic rash appears, the virus may have already spread to others.
This is why early recognition and prevention play such an important role in protecting families and communities.
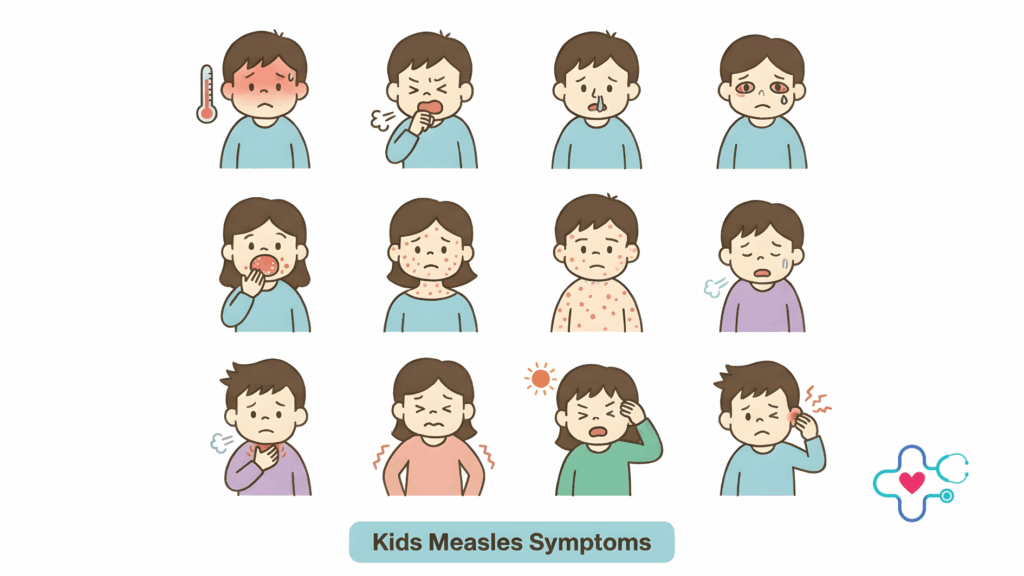
Early Measles Symptoms Parents Often Miss
Many parents associate measles with a rash — but the rash comes later.
In the early stage, measles often looks like a severe cold or flu. Symptoms may include:
- High fever, often rising quickly
- Cough
- Runny nose
- Red, watery, or irritated eyes
- Fatigue, irritability, or decreased appetite
Because these symptoms are common with many viral illnesses, measles can be difficult to identify at first. A key difference parents often notice is how sick their child looks and feels, especially when fever is high and persistent.
When the Rash Appears
The measles rash typically develops three to five days after fever begins. It usually:
- Starts on the face or hairline
- Spreads downward to the neck, trunk, arms, and legs
- Appears as flat red spots that may merge together
If your child develops fever followed by a spreading rash, or symptoms seem to worsen instead of improve, it’s important to contact a medical provider.
Why Measles Can Be Serious for Children
While many children recover from measles, it is not always a mild illness. Some children are at higher risk for complications, including:
- Infants under 12 months
- Children who are not fully vaccinated
- Children with asthma or chronic medical conditions
- Pregnant individuals and immunocompromised family members
Complications can include ear infections, dehydration, pneumonia, and in rare cases, serious neurologic issues. This is why prompt guidance and careful monitoring are important, even if symptoms seem manageable at first.
How Parents Can Protect Their Children From Measles
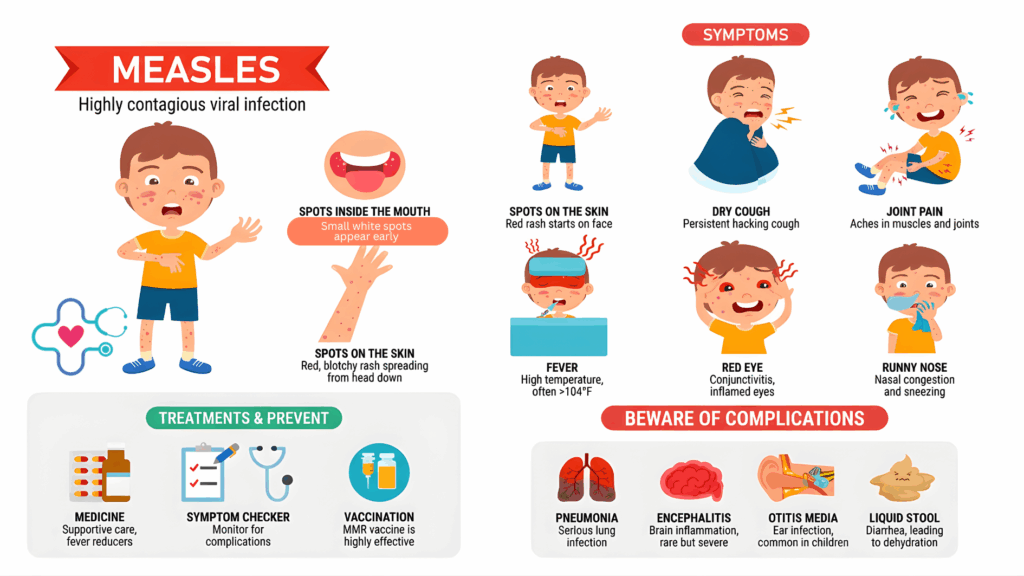
MMR Vaccination
The MMR (measles, mumps, rubella) vaccine is the most effective way to prevent measles. Two doses provide strong, long-lasting protection and significantly reduce the risk of severe illness and complications.
If you’re unsure whether your child is up to date on vaccinations or have questions about timing, a pediatric provider can help review your child’s immunization history and answer concerns.
Reducing Exposure
During times of increased measles activity:
- Avoid close contact with anyone who has fever and rash symptoms
- Be cautious in crowded indoor settings when possible
- Notify your healthcare provider if your child may have been exposed
Protecting High-Risk Family Members
If your household includes infants, pregnant individuals, or people with weakened immune systems, extra care is important. Keeping eligible family members vaccinated and limiting exposure to illness helps protect those most vulnerable.
When to Call Before Coming In
Because measles spreads so easily, calling ahead before visiting urgent care is essential.
Please contact a medical provider first if your child has:
- Fever along with a rash
- Known exposure to someone with measles
- Symptoms and is not fully vaccinated
Calling ahead allows our team to prepare appropriately and helps protect other children and families in our care.
Seek urgent or emergency care immediately if your child experiences:
- Trouble breathing or fast, labored breathing
- Extreme sleepiness, confusion, or difficulty staying awake
- Signs of dehydration such as very dry mouth, no tears, or minimal urination
- A very high fever that does not respond to medication
You never have to make these decisions alone. We are always here to help guide you.
Parents searching for measles treatment in Winchester can visit Night Watch Urgent Care for timely pediatric assessment and guidance.
We help families decide whether symptoms can be monitored safely at home or require in-person evaluation, while keeping safety and infection control a priority.
CATEGORY
2/06/2026
POSTED
Why Kids in the Kitchen = Burns, Cuts & Urgent Care Visits
Your 7-year-old: “Can I help make dinner?”
You: “Sure! You can stir the pasta.”
Five minutes later: They grabbed the hot pot handle. With their bare hand.
Now you’re at Night Watch.
Why Kids Get Hurt in the Kitchen
Children LOVE helping in the kitchen. They also:
- Don’t understand cause and effect yet
- Move unpredictably
- Have poor impulse control
- Forget instructions immediately
- Get excited and rush
- Touch things they’re told not to touch
Translation: They’re injury magnets.
The Most Common Kid Kitchen Injuries
1. Burns (Top of the List)
🍳 Hot pots and pans
Kid reaches for something, touches hot cookware. Second-degree burns on palms/fingers.
💧 Boiling water
Spills, splashes, or they pull pot handle. Scalding burns on hands, arms, chest.
🔥 Stove burners
“I didn’t know it was still hot.” Electric burners stay hot for LONG time after turning off.
🍕 Ovens
Reaching in, arm touches rack or door. Burns in stripes across forearm.
2. Cuts
🔪 Knife accidents
“I was just trying to help cut the vegetables.” Deep lacerations on fingers.
🥫 Can lids
Sharp edges on opened cans. Kids don’t realize how sharp they are.
🍷 Broken glass
Drop a glass, try to pick it up. Lacerations on hands.
3. Other Injuries
- Fingers smashed in drawers/cabinets
- Falls from standing on chairs/stools
- Slipping on spills
- Getting hit by falling pots/utensils
When to Bring Them to Night Watch
For Burns:
- Blisters larger than a quarter
- Burns on face, hands, feet, or genitals
- White or charred skin
- Child is in severe pain
- Burn larger than child’s palm
For Cuts:
- Won’t stop bleeding after 10 minutes
- Deep cut (gaping edges)
- On face, hands, or over joints
- Child can’t move fingers normally
- Numbness or tingling
What We Do at Night Watch
We specialize in pediatric care. We know how to:
- Keep kids calm during treatment
- Properly assess burn depth in children
- Apply child-friendly dressings
- Give age-appropriate pain relief
- Educate parents on wound care
Teaching Kitchen Safety
Before they help in the kitchen:
The Rules (Repeat Often)
- “Hot means DON’T TOUCH”
- “Knives are not toys”
- “Ask before touching anything”
- “If you drop something, tell a grown-up”
- “Walk, don’t run in the kitchen”
Safe Tasks by Age
Ages 2-4:
- Washing produce, tearing lettuce, mixing cold ingredients
Ages 5-7:
- Measuring, pouring, stirring, setting table, using butter knife
Ages 8-10:
- Peeling vegetables, using microwave, cracking eggs, using hand mixer
Ages 11+:
- Using sharp knives WITH SUPERVISION, basic stove use, following recipes
Creating a Safer Kitchen
- Turn pot handles inward (away from edge where kids can grab)
- Use back burners when possible
- Keep sharp objects in drawers/cabinets kids can’t reach
- Store cleaning products up high or locked
- Teach safe knife handling (claw grip, cut away from body)
- Supervise constantly — they’re quick!
First Aid at Home
For Minor Burns:
- Run under cool (not ice cold) water for 10-20 minutes
- Cover with clean, dry cloth
- Give age-appropriate pain relief
- Don’t pop blisters
For Minor Cuts:
- Apply direct pressure for 10 minutes
- Clean with soap and water
- Apply antibiotic ointment
- Cover with bandage
👨🍳 “I can help!” (Famous last words before urgent care)
We’ll patch them up and teach you safer cooking.
CATEGORY
1/31/2026
POSTED
“Pink Eye Going Around—AGAIN!”
You see the notification on your phone:
“FYI – multiple cases of pink eye in Mrs. Johnson’s class.”
Your heart sinks. Your kid is in Mrs. Johnson’s class.
Sure enough, the next morning: “Mom, my eye feels weird.”
Here we go again.
📚 Why Schools Are Pink Eye Breeding Grounds
January = peak pink eye season in schools. Here’s why:
- Back from winter break – mixing germ pools from different families
- Cold/flu season – viral pink eye often accompanies colds
- Indoor classroom time – less fresh air, more shared surfaces
- Kids touching EVERYTHING – then rubbing their eyes
- Close contact – circle time, group projects, lunch tables
One infected kid can spread pink eye to half the class in days.
What Parents Need to Know
It Looks Different Depending on the Type
VIRAL (most common in school outbreaks):
- Watery, clear tears
- Very red, very itchy
- Usually starts one eye, spreads to other
- May have runny nose, sore throat
BACTERIAL (needs antibiotics):
- Thick, goopy, yellow-green discharge
- Eyes crusted shut in morning
- More painful than viral
- Can spread to other eye
When to Bring Your Child to Winchester
Come in if:
- Eyes are red and producing discharge
- School requires doctor’s note before return
- Thick, colored goop (likely bacterial)
- Child complains of eye pain
- Vision seems blurry or affected
- Not improving after 3 days
- Infant or baby has pink eye (always needs evaluation)
What We Do at Night Watch
We specialize in pediatric care, and we see pink eye constantly this time of year:
- Quick examination to determine viral vs. bacterial
- Antibiotic eye drops if bacterial (prescribed on-site)
- School clearance notes so they can return
- Parent education on preventing spread to siblings
- Comfort measures for itchy, irritated eyes
🏠 Keeping It from Spreading at Home
You have multiple kids. How do you keep them ALL from getting it?
- Separate towels & pillows
- Wash hands constantly – especially after touching infected child’s face
- Change pillowcase daily
- Don’t let them share devices/tablets
- Disinfect high-touch surfaces – doorknobs, light switches, bathroom faucets
- Teach “don’t touch your eyes” (good luck)
- Wash infected child’s hands frequently
👶 Pink Eye in Babies
Infants with pink eye always need medical evaluation.
Why? Pink eye in newborns can indicate:
- Blocked tear duct (common, usually harmless)
- Bacterial infection (needs prompt treatment)
- In rare cases, serious infection requiring immediate care
If your baby (under 1 year) has red, goopy eyes, bring them in same day.
📅 When Can They Go Back to School?
Most schools require:
Bacterial pink eye: 24 hours after starting antibiotic drops + doctor’s note
Viral pink eye: When discharge has stopped and eyes are no longer red
We provide school clearance notes at your visit.
💡 Home Care Tips
While waiting for it to clear:
- Warm compress – helps loosen crusty discharge
- Gently wipe away discharge with clean, damp cloth (use once, wash)
- Cool compress – for itching relief
- No contact lenses until completely healed
- Skip eye makeup (and throw out old mascara after infection)
👁️ Pink eye is going around. We’ve seen it before. Get them diagnosed. Get them back to school.
CATEGORY
1/20/2026
POSTED
Why Your Kid’s Humidifier Is Still Making Them Sick
Your child has been coughing for two weeks.
Not all day – mostly at night. And in the morning. They wake up wheezing. Their chest sounds tight. They say it’s hard to breathe.
You’ve tried everything: cough medicine, honey, propping up their pillow. Nothing helps.
Then someone asks: “Do you run a humidifier in their room?”
Yes. Of course you do. The air is so dry. You’re trying to help.
“When’s the last time you cleaned it?”
…Oh.
🫁 How Dirty Humidifiers Affect Kids’ Lungs
Children’s respiratory systems are more vulnerable than adults’:
- Smaller airways = easier to inflame and obstruct
- Still-developing immune systems = less able to fight respiratory infections
- Breathe faster = inhale more contaminated air per breath
- Sleep in small rooms = higher concentration of airborne contaminants
When a humidifier sprays bacteria, mold spores, and mineral dust into the air, kids’ lungs take the biggest hit.
What We Seeing at Night Watch
Child comes in with:
- Persistent nighttime cough
- Wheezing
- Shortness of breath
- Sometimes fever
We test for flu, RSV, COVID – all negative. No strep. Lungs sound clear-ish. Oxygen levels normal.
Then we ask: “Do you run a humidifier?”
Almost always: Yes.
“When did you last clean it?”
Usually: Silence. Or “Um… a few weeks ago?”
Symptoms of Humidifier-Related Illness
Come to Night Watch if your child has:
- Nighttime cough that’s been going on for days/weeks
- Wheezing or difficulty breathing
- Complaints of chest tightness
- Symptoms worse at night, better during school
- Fever with respiratory symptoms
- Asthma suddenly harder to control
- Recurring respiratory infections
🫧 “But I Rinse It Every Week!”
Here’s the problem: rinsing isn’t cleaning.
What you need to do:
Daily
- Empty ALL water from tank and base
- Rinse thoroughly with clean water
- Dry with clean towel (don’t just refill wet tank)
Every 3 Days
- Fill tank with white vinegar
- Let sit 20-30 minutes
- Scrub with brush to remove mineral deposits
- Rinse thoroughly
Weekly
- Disinfect with 3% hydrogen peroxide OR diluted bleach (1 tsp per gallon water)
- Let sit 10-30 minutes
- Rinse VERY thoroughly (no chemical residue)
Always
- Use distilled or demineralized water ONLY
- Replace filters per manufacturer instructions
🔬 The Science: What’s Growing
Research shows dirty humidifiers harbor:
- Legionella bacteria (causes Legionnaires’ disease)
- Pseudomonas aeruginosa (respiratory infections)
- Mold spores (asthma triggers, allergic reactions)
- Endotoxins (inflammatory compounds)
- Mineral particles (lung irritation)
All of this gets turned into a fine mist and sprayed directly into your child’s face while they sleep.
What We Do at Night Watch
- Evaluate respiratory symptoms
- Rule out infections (flu, RSV, COVID, pneumonia)
- Provide breathing treatments if needed
- Assess for environmental triggers
- Give parents concrete steps to eliminate exposure
The Experiment
Try this:
- Deep clean your humidifier (or throw it out and buy a new one)
- OR stop using it entirely for one week
- See if symptoms improve
If your child’s cough gets better when the humidifier is off? That’s your answer.
Sometimes the solution is simpler than you think.
CATEGORY
1/16/2026
POSTED
When Holiday Pet Excitement Leads to Urgent Care
You got your kids the puppy they’ve been begging for. Christmas wish granted!
Day 1: Pure joy. Day 2: Lots of energy. Day 3: “Mom, the puppy bit me!”
You look at your child’s hand. There are teeth marks. It broke the skin. It’s starting to swell.
Wait… do puppies bite this much? Is this normal? Should you be worried?
Why Kids Get Bitten More
Here’s what most parents don’t realize: children are more likely to get bitten or scratched by pets than adults.
Why?
- They move unpredictably (running, jumping, shrieking with excitement)
- They’re at face level with small dogs and puppies
- They don’t read warning signs (ears back, growling, stiff body)
- They want to hug and squeeze (which animals often don’t like)
- They put their hands where puppies bite during play
And puppies? They explore everything with their mouths. Including your child.
When to Bring Your Child to Night Watch
Come in right away if:
- The bite or scratch broke the skin
- It’s on their face, hands, or near joints
- It’s a puncture wound (deep, narrow)
- Bleeding won’t stop after 10 minutes of pressure
- Signs of infection (redness, swelling, warmth, pus)
- You’re not sure if the pet is fully vaccinated
🐱 Cat Scratches: Tiny But Trouble
Got a kitten instead? Those needle-sharp claws can cause Cat Scratch Disease.
What is it? Bacterial infection from bacteria in cat saliva that gets on their claws. Can cause fever, swollen lymph nodes, and fatigue in children.
Symptoms appear 3-14 days after the scratch:
- Red bump or blister at scratch site
- Swollen lymph nodes (especially under arms or neck)
- Fever
- Your child feeling tired or unwell
Cat scratches need treatment. Don’t ignore them.
Teaching Kids to Be Safe with New Pets
Prevention is key. Teach your children:
- “Gentle hands” No pulling, grabbing, or squeezing
- “No face kisses” Keep faces away from puppy mouths
- “Let sleeping pets lie” Don’t wake or startle them
- “No hands in mouth” Use toys for play, not fingers
- “Back away if scared” If the pet seems upset, give space
- “Tell a grown-up” Always report bites/scratches immediately
How We Help at Night Watch
At Night Watch, we treat animal bites and scratches in children regularly:
- Gentle, thorough wound cleaning
- Child-friendly evaluation (checking for nerve/tendon damage)
- Stitches if needed (with numbing medicine first)
- Antibiotics to prevent infection
- Parent education on wound care and pet safety
🏡 What to Do at Home Immediately
If your child gets bitten or scratched:
- Wash the wound immediately with soap and running water (5+ minutes)
- Apply pressure if bleeding
- Don’t panic (it scares your child more)
- Bring them to Night Watch for proper evaluation
🐾 New pets + excited kids = occasional injuries. We’re here when it happens.
CATEGORY
1/13/2026
POSTED
Flu season is here in Winchester, but with a few simple strategies, you can protect yourself and your family. Here’s what you need to know.
Get Your Flu Vaccine
Vaccination is the most effective way to prevent the flu. Everyone 6 months and older should get their annual flu shot, ideally in early fall before flu activity peaks. The vaccine takes about two weeks to become fully effective, so don’t wait.
Note: Children getting vaccinated for the first time may need two doses spaced four weeks apart.
Practice Good Hand Hygiene
Handwashing remains one of your best defenses against flu viruses. Encourage your kids to wash with soap and water for at least 20 seconds—singing a favorite song helps pass the time and makes it more enjoyable.
Key times to wash: before meals, after using the bathroom, after playing outside, and after coughing or sneezing.
Teach Proper Cough and Sneeze Etiquette
Show your children how to cough or sneeze into their elbow rather than their hands. This simple habit significantly reduces the spread of germs. Practice at home so it becomes automatic—many kids find it fun to “catch” their sneeze like a vampire in a cape.
Keep Sick Children Home
We know it’s challenging, but keeping feverish children home from school protects other children and gives your child time to recover. Kids should be fever-free for 24 hours without medication before returning to school or daycare.
Support Healthy Habits
A strong immune system makes a difference. Focus on the basics: adequate sleep, nutritious meals, regular physical activity, and plenty of water. These fundamentals help your child’s body fight off infections naturally.
Clean High-Touch Surfaces
During flu season, regularly wipe down frequently touched items like doorknobs, light switches, tablets, and toys. You don’t need to deep-clean constantly—just focus on these hotspots where germs tend to linger.
When to Contact Us
Most children recover from the flu at home with rest and fluids. However, call our office if your child has:
- Difficulty breathing or rapid breathing
- High fever over 104°F or fever lasting more than 3-4 days
- Signs of dehydration (no tears when crying, significantly decreased urination)
- Symptoms that improve then suddenly worsen
- Any concerns that something isn’t quite right
Trust your instincts—remember, you know your child best.
Stay Prepared, Not Worried
Flu season is manageable with the right approach. Get vaccinated, maintain good hygiene, keep sick kids home to rest, and support healthy habits. That’s really the foundation of flu prevention.
If your family does get sick despite your best efforts, remember that rest, comfort, and time usually do the trick and your Night Watch Winchester team is here to help if you need us.
CATEGORY
11/17/2025
POSTED
Learn how to keep your kids safe in Winchester’s summer heat! Tips from Night Watch Pediatric Urgent Care to beat dehydration & sunburn.
Whether you’re visiting Jim Barnett Park or camping in the Shenandoah Valley, Winchester summers mean outdoor fun. But our region’s heat can lead to dehydration and tick bites — here’s how to keep kids safe.
Tips:
√ Hydrate well for day trips & park visits
√ Use insect repellent & do tick checks after camping
√ Know signs of dehydration: dry mouth, no tears, fatigue
√ Keep sunscreen handy for outdoor sports
√ Carry a first aid kit in the car
When to Visit Us: For dehydration, heat exhaustion, or tick bite concerns, our kid-friendly urgent care is here evenings & weekends. IV fluids available for fast recovery.
Visit Night Watch Pediatric Urgent Care in Winchester, VA — we’re ready to help your family stay safe all summer.
CATEGORY
7/10/2025